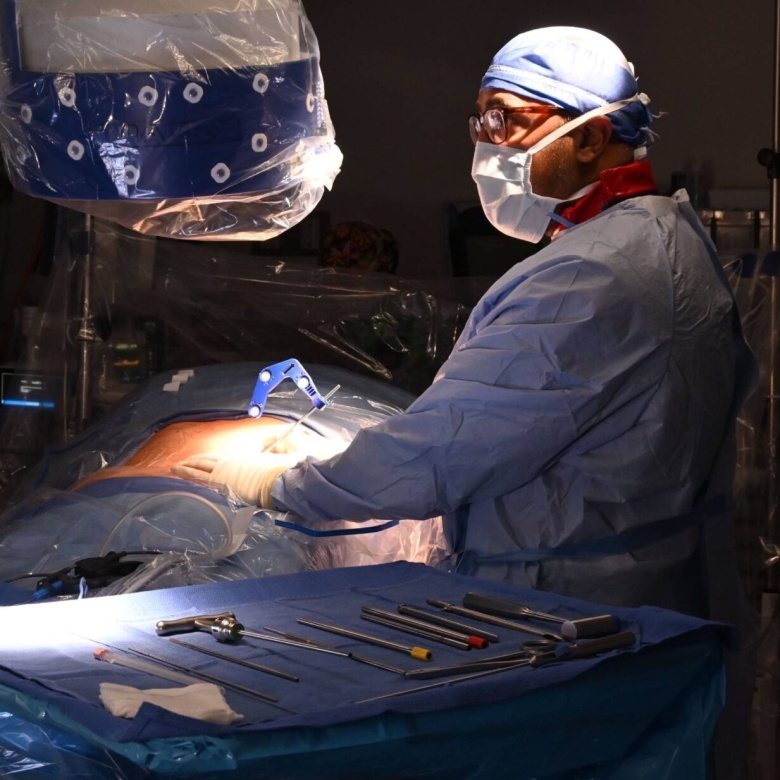
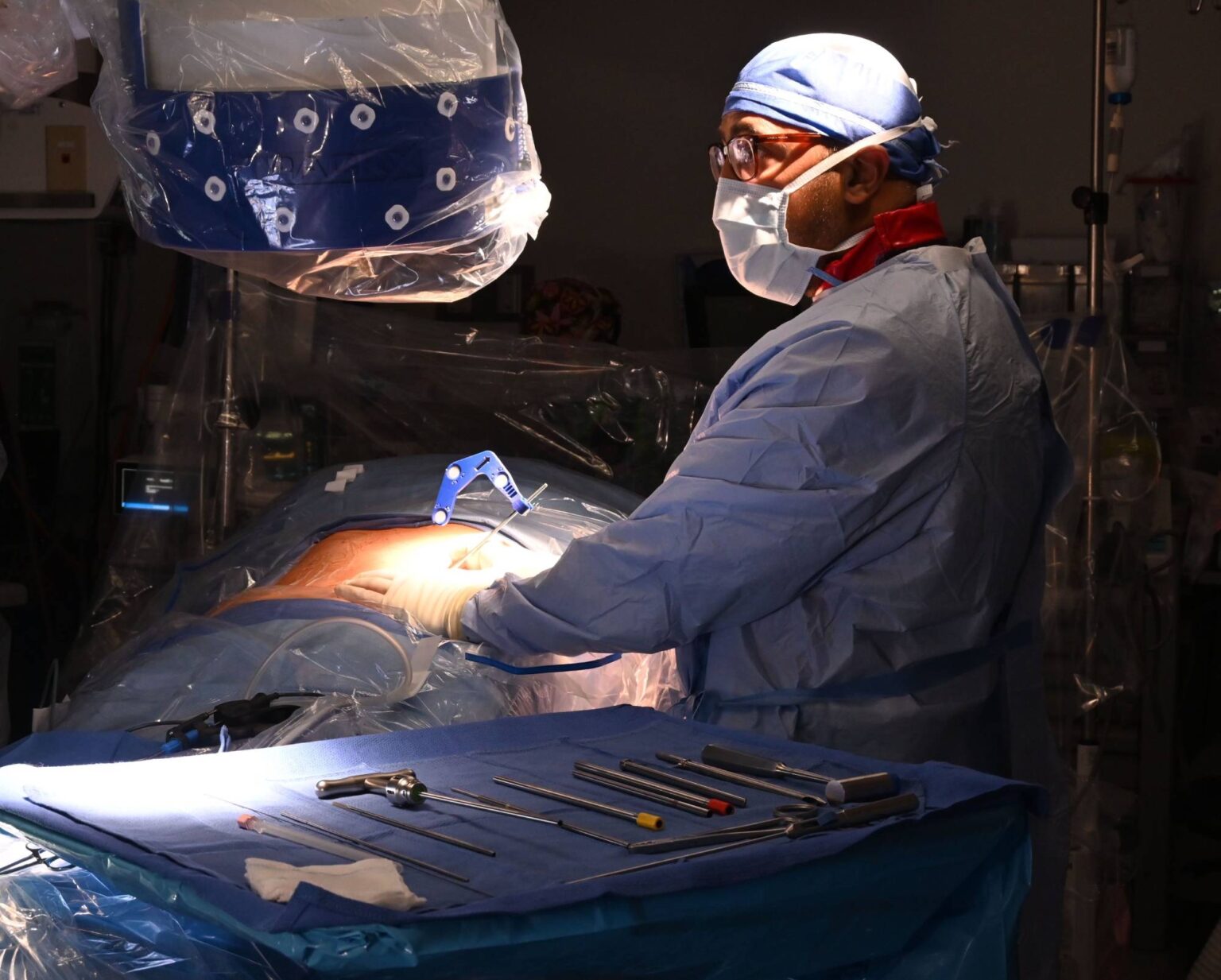
Over the past decade, minimally invasive spine surgery (MISS) has evolved from a niche alternative to a mainstream standard of care, driven by rapid advances in imaging, instrumentation, and digital navigation. At the core of contemporary MISS is the endoscopic ”spine camera,” a high definition, 30 degree optics system that can be introduced through a 5 to 10 mm working channel to visualize disc material, facet joints, and neural elements with unprecedented clarity. Coupled with specialized tubular retractors and expandable ”micro cannulas,” surgeons can now perform discectomies, foraminotomies, and even lumbar interbody fusions through incisions as small as 1 cm, dramatically reducing muscle disruption and postoperative pain.
Three-dimensional intra operative navigation, once limited to orthopedic trauma, now integrates seamlessly with fluoroscopic or O arm imaging to provide real time, sub millimeter localization of pedicle screws, cages, and biologic implants. When paired with robotic assistance—such as the Mazor X or ROSA platforms—these systems translate pre operative CT plans into precise, reproducible trajectories, decreasing screw malposition rates to below 2 % in most series. Augmented reality (AR) headsets further enhance the surgeon’s situational awareness by overlaying virtual anatomy onto the patient’s body, allowing for ”see through” guidance without diverting attention to external monitors.
Biologic adjuncts have also matured. Injectable calcium phosphate cements and porous titanium mesh cages expand the surgeon’s toolbox for restoring disc height and promoting osseointegration, while regenerative approaches—stem cell laden hydrogels and growth factor rich platelet rich plasma—are being investigated to accelerate fusion and reduce scar formation. Moreover, real time electrophysiological monitoring, now standard in most MISS suites, safeguards neural structures during the limited exposure afforded by these techniques.
Collectively, these innovations translate into tangible clinical benefits: shorter hospital stays (often same day discharge), lower blood loss (often <100 mL), and faster return to work. Long term outcomes for degenerative lumbar disease treated with endoscopic or robot assisted MISS are comparable, and in some registries superior, to traditional open approaches, particularly regarding preservation of paraspinal musculature and reduction of adjacent segment degeneration. As imaging resolution, AI driven planning, and bioengineered implants continue to converge, the next frontier of Minimally Invasive Spine Surgery Near Me promises even greater precision, personalization, and patient centered recovery.
Three-dimensional intra operative navigation, once limited to orthopedic trauma, now integrates seamlessly with fluoroscopic or O arm imaging to provide real time, sub millimeter localization of pedicle screws, cages, and biologic implants. When paired with robotic assistance—such as the Mazor X or ROSA platforms—these systems translate pre operative CT plans into precise, reproducible trajectories, decreasing screw malposition rates to below 2 % in most series. Augmented reality (AR) headsets further enhance the surgeon’s situational awareness by overlaying virtual anatomy onto the patient’s body, allowing for ”see through” guidance without diverting attention to external monitors.
Biologic adjuncts have also matured. Injectable calcium phosphate cements and porous titanium mesh cages expand the surgeon’s toolbox for restoring disc height and promoting osseointegration, while regenerative approaches—stem cell laden hydrogels and growth factor rich platelet rich plasma—are being investigated to accelerate fusion and reduce scar formation. Moreover, real time electrophysiological monitoring, now standard in most MISS suites, safeguards neural structures during the limited exposure afforded by these techniques.
Collectively, these innovations translate into tangible clinical benefits: shorter hospital stays (often same day discharge), lower blood loss (often <100 mL), and faster return to work. Long term outcomes for degenerative lumbar disease treated with endoscopic or robot assisted MISS are comparable, and in some registries superior, to traditional open approaches, particularly regarding preservation of paraspinal musculature and reduction of adjacent segment degeneration. As imaging resolution, AI driven planning, and bioengineered implants continue to converge, the next frontier of Minimally Invasive Spine Surgery Near Me promises even greater precision, personalization, and patient centered recovery.